Meningitis and Teenagers: What Every Parent Needs to Know
Meningitis in teenagers can develop rapidly and early symptoms may resemble flu or a hangover. This guide explains the warning signs parents should know and when to seek urgent medical help.

In March 2026, an outbreak of meningitis among students in Canterbury, Kent, has brought a disease many parents thought was largely under control back into sharp focus. Two young people have died. More than thirty thousand students and staff are being contacted by public health authorities. Parents across the country are asking the same question: could this happen to my child? The honest answer is that it could. But knowledge changes outcomes. This post explains the information that actually matters.
This is not a post designed to frighten you. Fear is not useful. What is useful is understanding how meningitis behaves in teenagers, what the vaccination picture looks like for this age group, and exactly what you and your child should do if something feels wrong. That is what we will cover here.
If your teenager has a high fever, severe headache, stiff neck, sensitivity to light, confusion, difficulty waking, or a rash that does not fade when pressed with a glass, do not wait. Call 999 immediately or go straight to A&E. Time is critical.
For non-emergency concerns:
NHS 111 | Meningitis Now: 0808 80 10 388 | Meningitis Research Foundation: 0808 800 3344
What is meningitis and why does it matter?
Meningitis is inflammation of the meninges[1], the protective membranes surrounding the brain and spinal cord. It can be caused by viruses or bacteria. Viral meningitis is more common and usually less severe. Bacterial meningitis is rarer but far more dangerous. It can become life-threatening within hours without treatment.
The Kent outbreak involves meningococcal group B (MenB)[2], a bacterial strain caused by the bacterium Neisseria meningitidis. Bacterial meningitis can also cause septicaemia, or blood poisoning, which is just as dangerous as the meningitis itself. The two conditions often occur together.
Around one in ten cases of bacterial meningitis in the UK is fatal.[3] Those who survive can be left with serious long-term complications including hearing loss, limb damage, and brain injury. Speed of treatment is the single biggest factor in outcomes.
Why are teenagers particularly at risk?
According to Meningitis Now, one in four 15 to 19-year-olds carry meningococcal bacteria harmlessly at the back of their throats, compared with around one in ten of the general UK population.[4] Most people who carry the bacteria never become ill. But the bacteria can spread through close contact, including coughing, kissing, and sharing drinks, vapes, or food.
The environments teenagers inhabit make transmission easier. University halls of residence, sixth form common rooms, shared houses, and nightclubs all involve the kind of close, prolonged social contact that allows the bacteria to move between people. First-year university students face a particular spike in exposure because they are suddenly mixing with large numbers of new people from across the country, each carrying their own bacterial profile.
There is an additional challenge specific to this age group: the early symptoms of meningitis can closely resemble a bad hangover, flu, or a heavy cold.[5] Severe headache, vomiting, sensitivity to light, fever, and general malaise are common to all of these. A teenager who has been out the night before may dismiss early warning signs, and so might the people around them. This is one of the most important things parents can understand.
For a detailed explanation of meningitis types, vaccines and the current protection gap in the UK, read our in-depth meningitis guide.
The vaccination picture for teenagers: what you need to know
This is the area that has caused the most confusion in the current outbreak, so it is worth being precise.
MenACWY
The MenACWY vaccine protects against four strains of meningococcal bacteria: A, C, W, and Y. It is routinely offered to teenagers in secondary school (usually Year 9 or Year 10 in England), and is also available free to young people up to the age of 25 who missed it, including those starting university for the first time.[6] Uptake is generally good, running at around 70 to 75 per cent in recent school cohorts, though it has not fully returned to pre-pandemic levels.
MenB
The MenB vaccine is where the gap lies. Since 2015, MenB vaccination has been offered to babies as part of the routine NHS immunisation schedule.[7] This means that current teenagers and university students, who were born before the programme began, will not have received it as part of their routine childhood vaccines. The Kent outbreak has been confirmed as MenB.
The MenACWY vaccine your teenager received at school does not protect against MenB.
MenB vaccination is available privately for teenagers and adults at typically around £100 to £150 per dose, with a minimum of two doses required.[8] Meningitis Now has launched a campaign calling for MenB vaccination to be made available to all teenagers and young adults on the NHS, arguing that the current situation leaves an entire generation unprotected against the most common meningococcal strain in their age group.
Check your child's vaccination record for the following:
- MenACWY: offered in secondary school (usually Year 9 or Year 10 in England). Available free up to age 25 if missed. Speak to your GP.
- MenB: not routinely offered to this age group on the NHS. Available privately from GPs, travel clinics, and some pharmacies. Typically around £100 to £150 per dose; two doses required.
- Unsure about vaccination history? Check the NHS app, contact your GP, or ask at a travel clinic.
Vaccination reduces risk significantly but does not eliminate it entirely. Knowing the symptoms remains essential regardless of vaccination status.

Recognising the symptoms: what to tell your teenager and yourself
The symptoms of bacterial meningitis and meningococcal septicaemia can appear in any order, and not all of them will be present in every case. This is what makes recognition genuinely difficult.
Early symptoms (which can resemble flu or a hangover)
- Severe headache
- High temperature (fever)
- Vomiting
- Sensitivity to bright light
- Muscle and joint pain
- Cold hands and feet despite fever
- Pale, mottled, or blotchy skin
- Difficulty waking or unusual drowsiness
- A general feeling of being very unwell, with symptoms worsening quickly
More serious symptoms (act immediately if these appear)
- Stiff neck (difficulty putting chin to chest)
- Severe sensitivity to bright light
- Confusion or disorientation
- Seizures
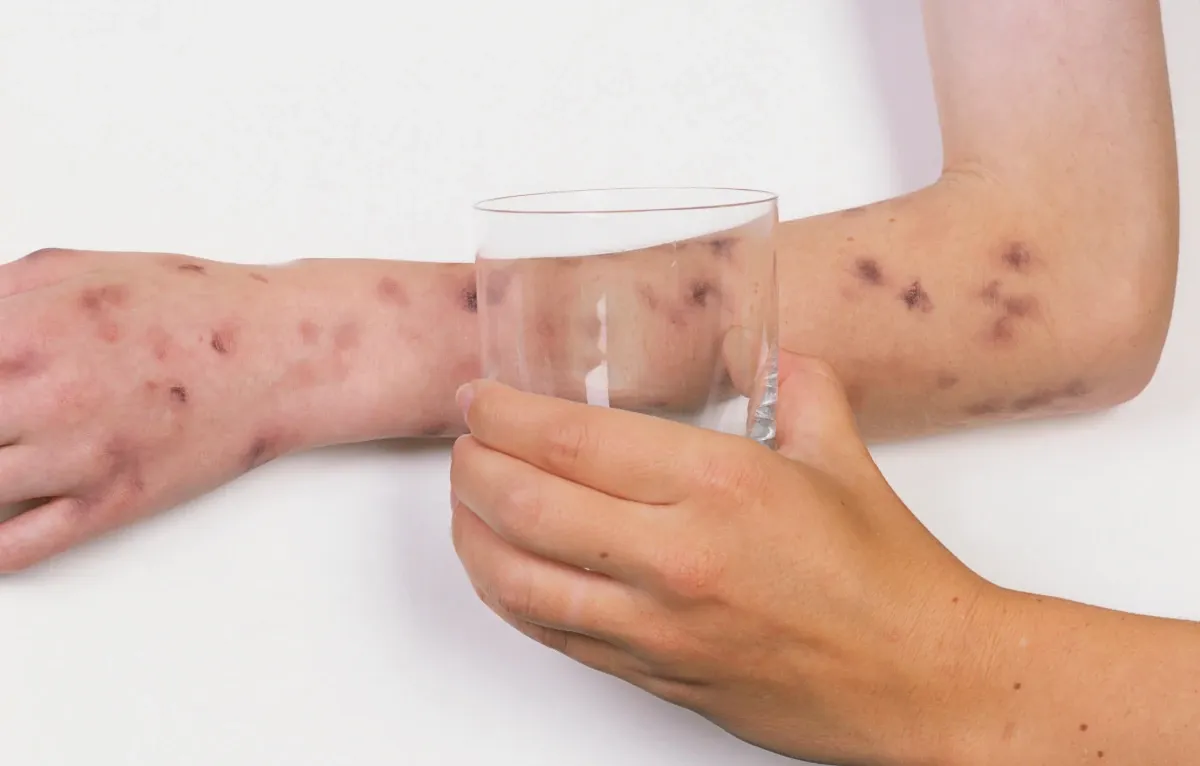
- A rash that does not fade when pressed with a glass (the 'glass test')
Press a clear glass firmly against the rash. If the rash does not fade under the pressure, this is a medical emergency. Call 999 immediately.
Important: not all cases of meningococcal disease produce a rash, and if a rash is present it often appears late in the illness. Do not wait for a rash before seeking help. The absence of a rash does not rule out meningitis.
Do not wait for a rash. It may appear late in the illness or not at all
The disease can progress from early symptoms to a critical condition in a matter of hours.[9] If your teenager is deteriorating rapidly, trusting your instincts and calling 999 is the right decision. You will not be wasting anyone's time.
What to do if you are concerned
If symptoms are mild or uncertain
Contact your GP or call NHS 111 (dial 111 or visit 111.nhs.uk). Describe the symptoms clearly. If things change or worsen, do not wait for a callback, call 999.
If symptoms are severe, rapidly worsening, or include a non-fading rash
Call 999 immediately or go directly to the nearest A&E. Do not drive yourself. Early antibiotic treatment is the single most important factor in survival and recovery. The sooner antibiotics are administered, the better the outcome.
If your child is at university and has been identified as a close contact
They may be contacted directly by UKHSA or their university and offered preventive antibiotics (prophylaxis). They should take these even if they feel well. If they believe they have been in close contact with a confirmed case but have not been contacted, they should go to their university health centre or call NHS 111 for advice.
If your teenager dismisses their own symptoms
This is a real practical challenge. Students may not want to worry you, may attribute their symptoms to a night out, or may simply feel embarrassed about seeking help. It is worth having a direct conversation now, before any concerns arise, about the difference between feeling rough after a late night and the kind of rapid, severe deterioration that warrants calling for help. Give them permission to seek help without worrying about your reaction.
What first aid training adds to this picture
First aid does not treat meningitis. There is no intervention a first aider can perform that replaces rapid hospital treatment. What first aid training does is change how people respond in high-pressure situations.
Someone with first aid training is more likely to act decisively when they see a friend deteriorating quickly. They are less likely to adopt a wait-and-see approach in a situation where hours matter. They recognise when a situation requires urgent professional help, and they are more comfortable making the call.
In a student environment where meningitis symptoms can be confused with a rough night, the difference between someone who acts quickly and someone who waits until morning can be the difference between full recovery and long-term harm.
- Check your teenager's vaccination records. MenACWY should be in there. MenB will not be there unless they had it privately.
- Talk to your teenager now about recognising symptoms, not when they are already unwell.
- Rapid deterioration is the key warning sign. If someone goes from feeling unwell to very unwell quickly, call 999.
- A rash that does not fade under a glass is a medical emergency. But a rash may not appear at all. Do not use its absence to reassure yourself.
- Early antibiotic treatment saves lives. Do not delay seeking help to see whether symptoms improve on their own.
If you want a deeper explanation of how meningitis develops and why symptoms can escalate so quickly, you can read our in-depth guide here.
Further information and support
The following organisations provide reliable, up-to-date information on meningitis and support for those affected by it.
- Meningitis Now: 0808 80 10 388 | meningitisnow.org
- Meningitis Research Foundation: 0808 800 3344 | meningitis.org
- UKHSA (UK Health Security Agency): gov.uk/ukhsa
- NHS 111: dial 111 or visit 111.nhs.uk
References
[1] NHS. Meningitis. Available at: https://www.nhs.uk/conditions/meningitis/
[2] UKHSA. Cases of invasive meningococcal disease notified in Kent. March 2026. Available at: https://www.gov.uk/government/news/cases-of-invasive-meningococcal-disease-confirmed-in-kent
[3] London School of Hygiene and Tropical Medicine. Rapid reaction: What is meningitis B? 17 March 2026. Available at: https://www.lshtm.ac.uk/newsevents/news/2026/rapid-reaction-what-meningitis-b
[4] Meningitis Now. MenB campaign data. Available at: https://www.meningitisnow.org
[5] UKHSA. Cases of invasive meningococcal disease notified in Kent. March 2026. Available at: https://www.gov.uk/government/news/cases-of-invasive-meningococcal-disease-confirmed-in-kent
[6] NHS. MenACWY vaccine. Available at: https://www.nhs.uk/vaccinations/menacwy-vaccine/
[7] NHS. MenB vaccine for children. Available at: https://www.nhs.uk/vaccinations/menb-vaccine-for-children/
[8] ITV News. What do we know about meningitis B and how serious is it? 17 March 2026. Available at: https://www.itv.com/news/2026-03-17/what-do-we-know-about-meningitis-b-and-how-serious-is-it
[9] NHS. Meningitis: symptoms and complications. Available at: https://www.nhs.uk/conditions/meningitis/symptoms/




